Ophthalmology ST1 Interview: 2026 Guide
If you’re considering applying for Ophthalmology ST1, this guide will provide everything you need to know about the application process, key recruitment dates and the interview format.
Ophthalmology ST1 is a competitive pathway. In 2025, there were 2,197 applications for just 102 posts, giving a competition ratio of 21.54. This means there were almost 22 applications for every post available. This is a big increase from 2024, when there were nearly 15 applicants for each post. With the competition only increasing, it’s essential that you prepare well for the interview and perform to the best of your ability.
Ophthalmology ST1 Key Dates
The 2026 recruitment dates for Ophthalmology ST1 are as follows:
| Stage | Date |
|---|---|
| Applications open | 23 October 2025 |
| Applications close | 20 November 2025 |
| Invitation to book MSRA expected no later than | 15 December 2025 |
| Multi-Specialty Recruitment Assessment (MSRA) | 6 — 19 January 2026 |
| Documentation upload window | 16 January — 2 February 2026 |
| Candidates invited to book an interview slot | 6 March 2026 |
| Interview date | 16 & 17 March 2026 |
| Feedback released | 19 March 2026 |
| Offers released by no later than | 24 March 2026 |
Ophthalmology ST1 Application
For 2026, the selection process consists of the following three components, which we will cover in more detail in the sections below:
Only the highest ranking 260 applicants will be invited to interview, so you must also ensure you meet the essential eligibility criteria outlined in the Ophthalmology ST1 person specification.
Following the interview, your performance in the evidence folder and online interview will be combined to give you an overall score, which is used to rank you against other candidates. The maximum score for each component is as follows:
- Evidence Folder – Maximum 50 points
- Online interview – Maximum 50 points
Doing well in the MRSA exam will get you that interview, and then your interview and evidence folder are key to get you that offer; targeting your revision over just a few months will help you achieve highly in the MSRA and interview!
Ophthalmology ST1 Evidence Folder
As mentioned above, you must submit an evidence folder as part of the selection process. This involves uploading documents to a specifically designed online portal to demonstrate your achievements within the set domains; for example, qualifications, prizes/awards and commitment to ophthalmology (e.g. electives/taster weeks). Your evidence folder will be scored against a set criteria for each domain.
For more information and a full breakdown of the evidence folder domains and scoring, please see our 2026 guide to the Ophthalmology ST1 Interview Evidence Folder.
Crucially, your evidence folder should be clearly laid out, following the mark scheme to the letter, as you have no opportunity to explain or present your contents. Therefore, it is vital that it is organised and everything that is worth points is easily navigable and scored for your benefit. Include only what directly earns points and remove unnecessary extras that could distract assessors.
There are a few ways to gain some last-minute marks if you haven’t already got them. For example:
- You can “design an educational course” via an e-learning tool, which you can put together in your local hospital.
- Alternatively, you can gain 0.5 points for simply completing a course like the Medibuddy Teach the Teacher course. If you prefer an interactive learning environment where you can actively engage with tutors and peers, we also offer Live Teach the Teacher Courses.
- In “commitment to ophthalmology”, if you haven’t already, you can ask your friendly local ophthalmologist to spend time with them in eye casualty (with a letter as evidence for points).
- There are also marks for the use of the EyeSi programme, which is a microsurgical simulator that junior trainees use, for example, in training for independent cataract surgery. Only a few units, such as Moorfields Eye Hospital, Western Eye Hospital and the Royal College of Ophthalmologists, have this simulator, and the best way to access these is to ask an ophthalmology trainee.
For more advice on structuring your evidence folder and using what you already have to maximise marks, check out our blog post on preparing your evidence folder.

Teach the Teacher Course by Medibuddy
This two-day CPD-accredited online course will earn you 12 CPD points on completion. It’s entirely flexible, so you can complete it in two days or multiple sessions over a longer period. On completion of the course, you’ll receive a certificate for your portfolio that is accredited for CCT, interviews and appraisals.
Find out moreOphthalmology ST1 Self-Assesssment
New for the 2026 recruitment round, candidates must complete a self-assessment as part of their application. This involves awarding yourself scores for your achievements across eight domains, using the official scoring framework published in the recruitment resources.
You’ll need to:
- Score yourself accurately against the criteria for each domain (maximum total: 47 points).
- Submit both components by the upload deadline on 2 February 2026:
- A completed proforma including your self-scores and brief notes describing the supporting evidence. This should be uploaded as the first document in your evidence folder.
- An online form submission, where you’ll enter only the scores.
It’s important that your scoring honestly reflects your achievements. Over-claiming or exaggeration can trigger a probity investigation; in serious cases, this may result in disqualification or referral to the GMC (though this is rare).
You must achieve a minimum self-assessment score of 19 points to progress in the selection process, regardless of your MSRA score. If your self-score falls below this threshold, it might be worth delaying your application until a future recruitment round.
Multi-specialty Recruitment Assessment (MSRA) Exam
The MSRA is a multiple-choice exam that is also taken by GP, radiology, emergency medicine and other specialty applicants. It consists of an SJT-type component and a general medical questions component.
The best advice for this is to do as much practice as possible. It is not a difficult exam, but you need to do reasonably well to simply get an interview. The cut-off score for interview will vary from year to year.
The 2026 exam will take place at Pearson Vue test centres, with the exact dates still to be confirmed Most applicants will spend months preparing for this exam, so we recommend you do the same to increase your chances of scoring well.
The Medibuddy adaptive MSRA question bank has been built with you in mind. Preparing for interviews and exams, working full-time and trying to maintain a work-life balance can be incredibly tough. We know, we have been through it ourselves!
Take your MSRA revision to the next level with our artificial intelligence powered, adaptive question bank
Our state of the art algorithms will help you progress faster than ever.
Our question bank has been designed using sophisticated AI-powered algorithms which help you prepare quickly and efficiently. Unlike regular question banks, our algorithms tailor learning specifically to you, as opposed to just giving you access to a huge database of questions. We won’t randomly give you questions; we will provide questions that will actually increase your exam score.
Practice is especially important in the clinical component and can also be useful in your interview. It is usually based on generic, GP-tailored medical knowledge, which is a useful refresher for some basic interview questions. Here is an example of a clinical question from our MSRA question bank.
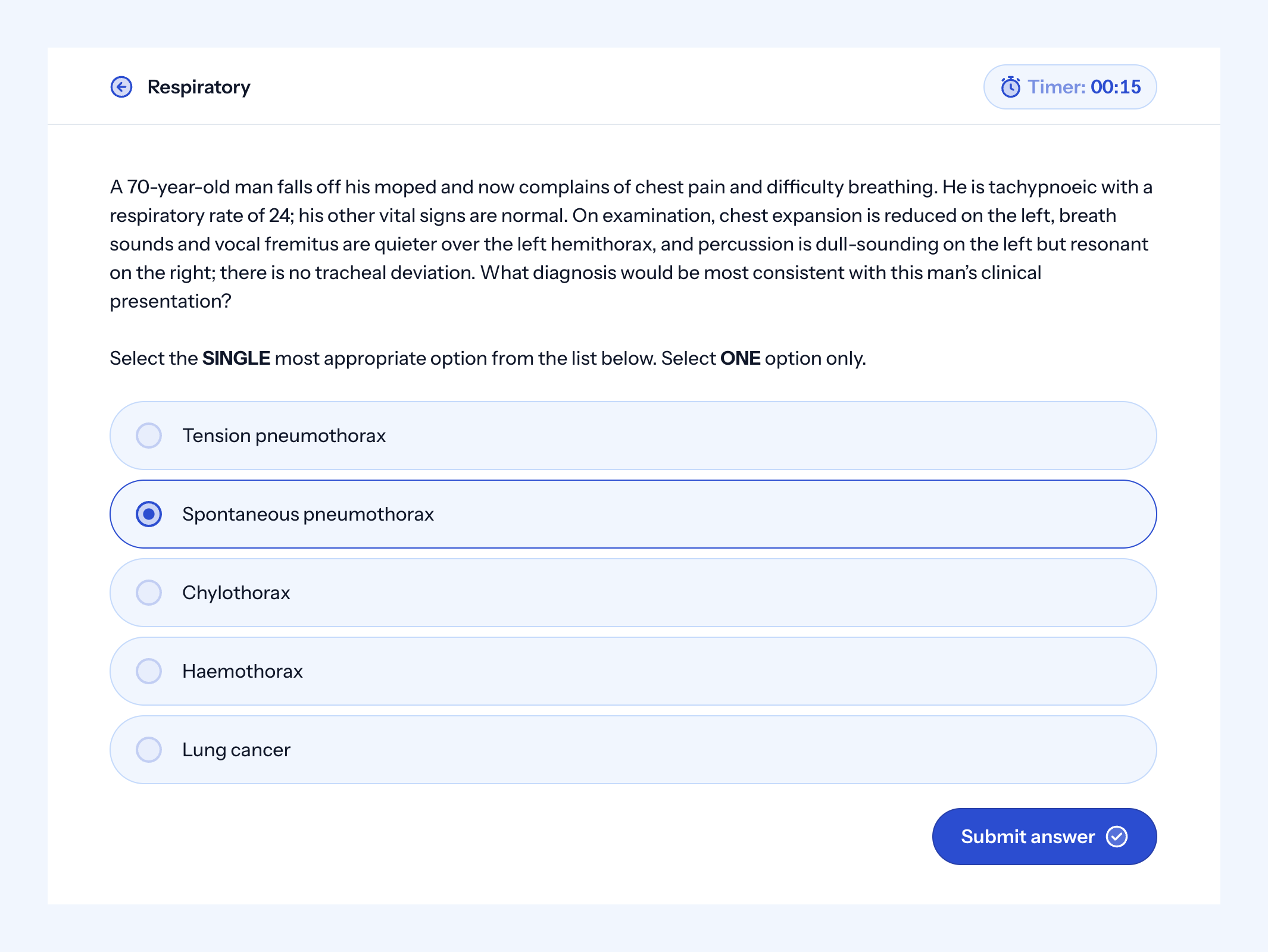
You can find out more about our question bank here.
Ophthalmology ST1 Interview Format
For 2026, the interview will have the following two components.
- Component 1: Assessment in the form of clinical knowledge
- Component 2: Assessment will be in the form of a medical consultation focusing on a difficult communication or ethical scenario
You will be invited to book your online interview if you meet the required MSRA score and rank as one of the top 260 applicants. Interviews are scheduled to take place between 16 & 17 March 2026.
Our question bank contains scenarios that mirror the Ophthalmology ST1 interview format, allowing you to perform well and score highly.
Before your interview, ensure you have a strong wi-fi connection, a good laptop camera and room lighting, and are familiar with Microsoft Teams. Ensure that you have tested this prior to your interview!
Each component involves a patient consultation with an actor and will be up to 10 minutes in length, but be sure to give 45 minutes for your interview, including identity checks, reading time, the assessment and debrief. You will be tested on your clinical knowledge and communication skills. As with previous face-to-face interviews, clinical scenarios and communication skills tend to be fairly realistic and based on real-life scenarios as an ophthalmologist that you would encounter in your clinic.
There could potentially be a wide range of different topics based on various themes. As a suggestion, do prepare to be familiar with the following scenarios as a starting point:
- Patient with decreased vision, with diabetic retinopathy/maculopathy. You explain to them what the disease is, how it affects vision, treatment options, lifestyle advice and diabetic control.
- Patient with glaucoma, with progressing visual field loss and inadequate eye pressure control. You need to advise them about treatment compliance and disease progression, and always remember to check a social history, e.g. driving – do they meet the driving standards? What do they do for a living?
- Angry patient: common scenarios involve previous misdiagnoses (or poorly explained diagnoses), cancelled/delayed appointments and treatments not working.
- Refractive surprise: patient after cataract surgery noticing much worse vision – how would you approach this and what investigations would you instigate?
- Breaking bad news: for example, incidental finding of ocular metastasis. How would you begin a difficult consult like this? What does the patient know? What are your suggested next steps?
To progress to the offers stage, candidates must achieve a minimum score of 40% in the interview assessment.
We have various example questions within our question bank, written by current ophthalmology trainees who ranked in the top 5% of the application cycle, and the picture below gives you a flavour of what to expect when you purchase.
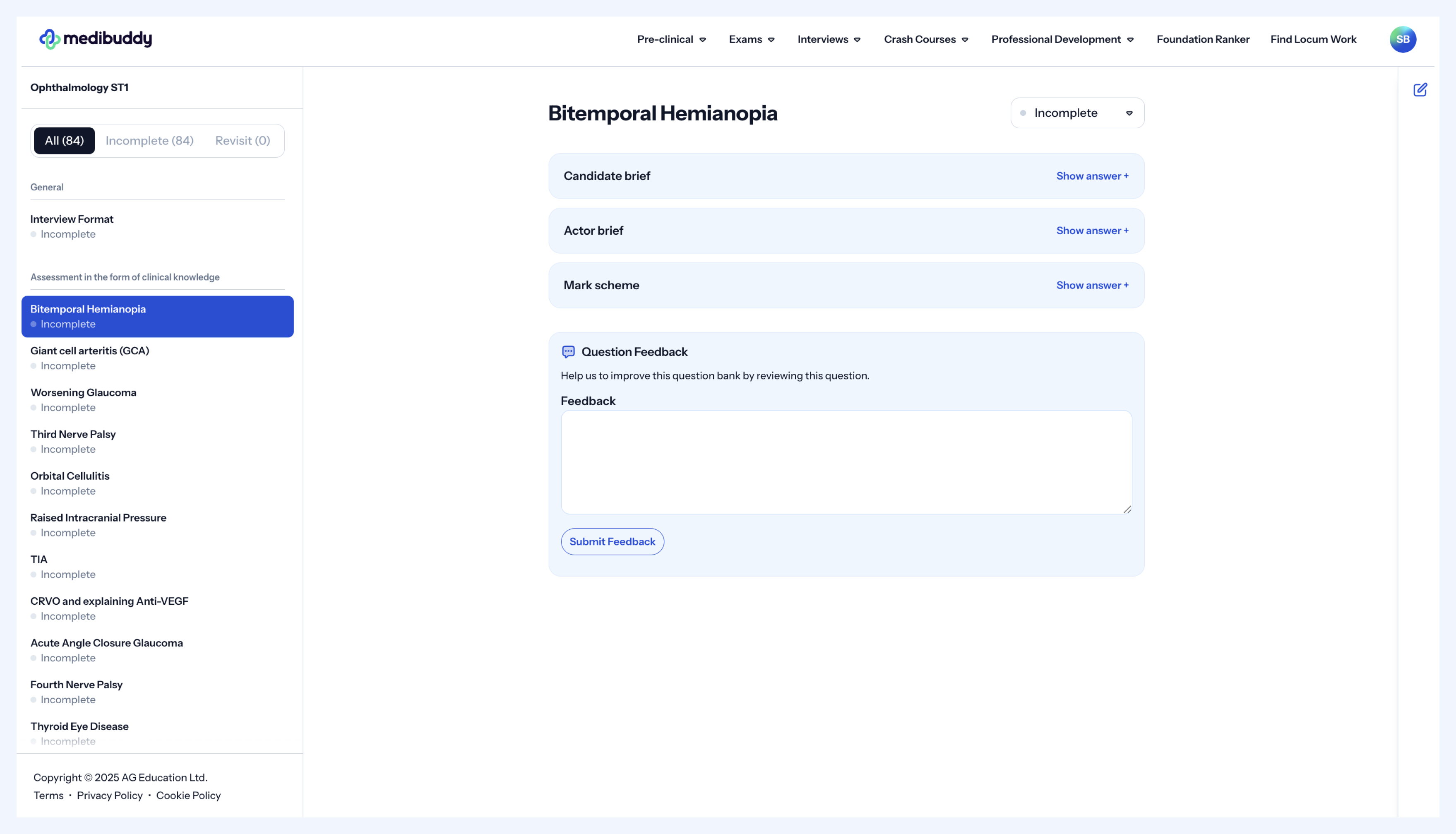
Although there are no specific QIPP/Audit stations this year, these are overlapping and very relevant themes in ophthalmology in general. Therefore, we have left these scenarios in our question bank for reference, and we recommend you read through these scenarios to familiarise yourself with cases like this and beyond. It is always easier if you have encountered real-life situations like this in a clinical setting, so do try to gain some prior ophthalmology clinical experience if you can. Use your taster week wisely!
Final tips
- Get started as early as you can! Get your evidence folder in order, as it takes a lot longer than you expect.
- Put time aside to practise for the MRSA exam and do lots of questions.
- Prepare for the online interview as you would with real-life OSCE stations. Practise with a partner online on Microsoft Teams for familiarity.
- Remember, you are scored stringently with a mark scheme, and almost half your battle is done when you submit your evidence folder.
- Coming across as well-mannered and thoughtful is always important at any interview and especially on a video call.
Good luck!
Take your subscriptions with you
Our mobile app allows you to access your interview and exam question banks wherever you are.